The add value of laboratory diagnostics: the many reasons why decision-makers should actually care
The landscape of laboratory medicine, within the increasingly complexity of the third millennium healthcare, is multifaceted (1). On one hand, the core of our daily work as laboratory professionals can be straightforwardly summarized in a pivotal sentence captured from the preface of Tietz’s Applied Laboratory Medicine, “Laboratory medicine plays an integrated role in the diagnosis, prognosis, treatment, and long-term management of disease”. Most of us would hence agree that, throughout its long history, laboratory medicine has represented an essential and virtually unavoidable milestone for the clinical decision making. This influential statement is supported by a bout of evidence clearly attesting that laboratory testing generates fundamental, “clinically-usable” information for management of most human pathologies and for the progress of science and medicine (2). There are also some notable (and positive) exceptions to this rule, since laboratory testing is now the one and only means for the diagnosis of certain diseases. Cardiac troponins testing, by using the novel high-sensitivity immunoassays, is the benchmark for diagnosing non-ST elevation myocardial infarction (NSTEMI), which now represents up to 60–70% of all cases of acute coronary syndromes (3). Molecular testing is also the core for diagnosing monogenetic disorders (4), whilst the personalized treatment of many cancers is now profoundly based on results of specific diagnostic tests (i.e., Her2/neu status in breast cancer) (5). Even diabetes mellitus, one of the most common human disorders, cannot be diagnosed without measurement of fasting plasma glucose or glycated hemoglobin (HbA1c) (6).
Albeit the over millenary history of laboratory medicine has finally contributed to entrench a positive culture on how this clinical branch is perceived by its many stakeholders, a number of challenges are plaguing the efficiency, even the outliving, of our profession. These include increasing complexity and volume management, enhanced demand of care, liability, inappropriateness, professional decline, direct-to-consumer testing, reimbursement policies and, last but not least, shortage of public funding. This last aspect is especially concerning, since over 50% of the budget of a medium-sized public laboratory actually relies on costs for instrumentation and reagents, so paving the way to some important reflections on the future of our discipline.
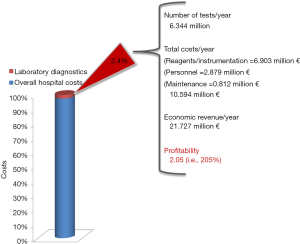
The first standpoint, that needs to be reaffirmed, is that the overall cost of laboratory testing is a drop in the ocean of the global healthcare expenditure. Recent statistics indicates that laboratory diagnostics contributes for only 1.4–2.8% to the overall balance of most national healthcare services around the world (7). These figures are globally in accordance with those calculated for a medium European public laboratory (Figure 1). Nevertheless, when the number of tests and their related costs are compared to the overall economic revenue calculated according to local reimbursement policies, the conclusion is that laboratory diagnostics actually erodes less than 2.5% of the total hospital expenditures, but ensures a profitability exceeding 300%. Obviously, this figure only considers costs for consumable and reagents, but when even total costs are included in the calculation (i.e., personnel and maintenance), the profitability remains well above 200% (Figure 1).
According to the prestigious journal Forbes (8), the top five most profitable worldwide industries include the generic pharmaceutic industry (30% net profit margin), followed by investment (29.1% net profit margin), tobacco (27.2% net profit margin), internet software/services (25% net profit margin) and biotechnology (24.6% net profit margin). Realistically, public clinical laboratories can hence ensure a net profit margin that is nearly 7-fold higher than whatever other industry, and would actually be approximately 10-fold larger than banks and information technology (both 23% net profit margin). Now, imagine to bring these figures to some experts of human capital management. No doubts, they will remain simply… fascinated. Notably, the impact of some capital costs (i.e., rent or purchase of buildings, national or local taxes) is virtually null for public laboratories, so that it should not surprise that the return of investment will be more favorable than for other industries. Nevertheless, this aspect does not actually overturn the former concept that laboratory medicine is indeed profitable for public hospitals and for the healthcare system as a whole, especially in those countries were public healthcare coverage is lower and/or insurance coverage is vast. To put this simply, laboratory diagnostics is a high-profitably enterprise (9).
Albeit laboratory medicine largely contributes to accountable care, this discipline has now become a prime target for cuts. While most public hospitals are still struggling to reach a break even and stay afloat, public laboratories only receive a fraction of what they bill, but are largely contributing to generate economic revenues that will ultimately contribute to offset the hospital losses. It is also quite bizarre that some credible, evidence-based efficiency analyses are completely overlooked while planning consolidation policies and scale economy (10). In view of this, whatever profitability analyst would consider quite masochistic to kill the golden goose. This springs to mind the question about why many decision-makers are still placing laboratory medicine in the firing line, by imposing huge economic constraints? Maybe because laboratory budgets are much more transparent than those of other healthcare disciplines [most often expressed in terms of diagnosis related groups (DRGs)], and it is hence much simpler to cut what you can precisely measure? Or maybe because laboratory medicine is still regarded as a commodity by many decision-makers and hospital administrators, and there is poor consciousness (if any…) about the negative consequences on the daily managed care from limiting diagnostic testing? Or, even worse (and this is our responsibility), because we have been unable to promote ourselves, and our essential activity, like many other clinical colleagues more efficiently do?
Last but not least, quality of testing is another foremost aspect (11). Cutting down the budgets of tenders will bring modest instrumentation and poor reagents into the laboratory. Quality does not come for free, and decision-makers should have already learnt that each money spent on quality will bring many savings afterwards as a consequence of a more efficient or timely diagnostic support and a lower risk of harm for the patients.
The role of laboratory managers has consistently changed over the last decades. Clinical and technical background is no longer sufficient, since the time spent in the laboratory is now increasingly committed to organizational, administrative and economic concerns. Although the relationship between costs, revenues and profits is indeed straightforward for in vitro diagnostic testing, many laboratory professionals are still struggling to keep their public labs afloat. This is quite inexplicable and unwarranted from both a clinical and a genuinely economic perspective. Our best weapon to reverse this trend is knowledge dissemination. In the era of personalized (laboratory) medicine (12), decision-makers will need a wealth of knowledge that laboratory medicine is not a deadwood, but is probably the key for a patient-centered and sustainable future of health care.
Acknowledgments
Funding: None.
Footnote
Conflicts of Interest: Both authors have completed the ICMJE uniform disclosure form (available at http://dx.doi.org/10.21037/jlpm.2017.12.07). Giuseppe Lippi serves as the unpaid Editor-in-Chief of Journal of Laboratory and Precision Medicine from November 2016 to October 2021. The authors have no other conflicts of interest to declare.
Ethical Statement: The authors are accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Open Access Statement: This is an Open Access article distributed in accordance with the Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License (CC BY-NC-ND 4.0), which permits the non-commercial replication and distribution of the article with the strict proviso that no changes or edits are made and the original work is properly cited (including links to both the formal publication through the relevant DOI and the license). See: https://creativecommons.org/licenses/by-nc-nd/4.0/.
References
- Plebani M. Quality in laboratory medicine: 50 years on. Clin Biochem 2017;50:101-4. [Crossref] [PubMed]
- Lippi G, Plebani M. Laboratory medicine does matter in science (and medicine)… yet many seem to ignore it. Clin Chem Lab Med 2015;53:1655-6. [Crossref] [PubMed]
- Roffi M. 2015 ESC Guidelines for the management of acute coronary syndromes in patients presenting without persistent ST-segment elevation: Task Force for the Management of Acute Coronary Syndromes in Patients Presenting without Persistent ST-Segment Elevation of the European Society of Cardiology (ESC). Eur Heart J 2016;37:267-315. [Crossref] [PubMed]
- de Koning TJ, Jongbloed JD, Sikkema-Raddatz B, et al. Targeted next-generation sequencing panels for monogenetic disorders in clinical diagnostics: the opportunities and challenges. Expert Rev Mol Diagn 2015;15:61-70. [Crossref] [PubMed]
- Nicolini A, Ferrari P, Duffy MJ. Prognostic and predictive biomarkers in breast cancer: Past, present and future. Semin Cancer Biol 2017; [Epub ahead of print]. [Crossref] [PubMed]
- American Diabetes Association. 2. Classification and Diagnosis of Diabetes. Diabetes Care 2017;40:S11-24. [Crossref] [PubMed]
- Lippi G, Plebani M. Laboratory economics. Risk or opportunity? Clin Chem Lab Med 2016;54:1701-3. [Crossref] [PubMed]
- Chen L. The Most Profitable Industries In 2016. Last access, 8 December 2017. Available online: https://www.forbes.com/sites/liyanchen/2015/12/21/the-most-profitable-industries-in-2016/#3849a69c5716
- Plebani M. Clinical laboratories: production industry or medical services? Clin Chem Lab Med 2015;53:995-1004. [Crossref] [PubMed]
- Barletta G, Zaninotto M, Faggian D, et al. Shop for quality or quantity? Volumes and costs in clinical laboratories. Clin Chem Lab Med 2013;51:295-301. [Crossref] [PubMed]
- Plebani M. Towards a new paradigm in laboratory medicine: the five rights. Clin Chem Lab Med 2016;54:1881-91. [Crossref] [PubMed]
- Lippi G, Bassi A, Bovo C. The future of laboratory medicine in the era of precision medicine. J Lab Precis Med 2016;1:7. [Crossref]
Cite this article as: Lippi G, Plebani M. The add value of laboratory diagnostics: the many reasons why decision-makers should actually care. J Lab Precis Med 2017;2:100.